Comprehensive Eye Health Exams
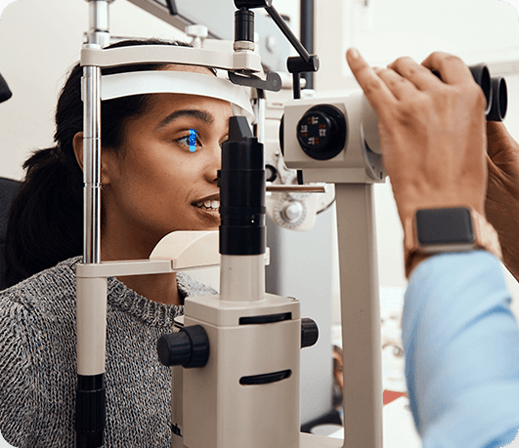
Our comprehensive eye health exams are so much more than a routine eye checkup and a prescription update! We take a complete and thorough look at your total eye health and vision to ensure there aren’t any developing issues or conditions. These eye health exams will help us make sure that your eyes are functioning properly, and your vision is as clear as possible!
Pediatric Eye
Health Exams
We work to protect the eyes of everyone in your family, including the littlest ones! Pediatric eye health exams help us identify conditions that are more common in children, so both you and your little one can feel confident in their eyesight and overall eye health!
Contact Lens
Exams and Fittings
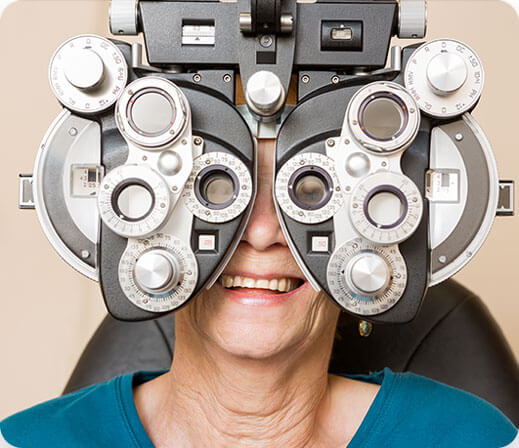
Unlike eyeglasses, contact lenses sit directly on the eye as opposed to in front of it. This means that a precise fit isn’t just important for comfort — it’s required for clear vision! During our contact lens exams, we match the correct lens to your vision needs and lifestyle and then walk you through proper ways to safely put them in your eyes.
Bringing Families in Our Communities
Clear Vision for over 80+ years
Eye Disease Management
When it comes to your eyes, detecting issues and diseases early is a critical part of protecting your vision. If we detect anything during a comprehensive eye health exam, our experts will tailor a treatment plan to meet your eyes’ specific needs.
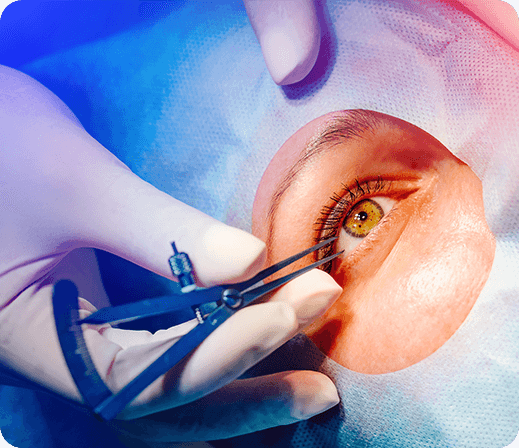
Surgical Co-Management
We stand by our patients every step of the way, which means we’ll also be by your side if you need cataract, LASIK, or glaucoma surgery. We work with trusted partners throughout Illinois and will refer you to one in your community if you need any of these procedures. We’ll make sure your surgeon knows your eyes as well as we do before the surgery, and then we’ll walk you through your recovery!
Testimonials
Our Convenient Locations
We have an 80+ years legacy in Illinois for providing top-quality contacts and contact lens exams to families like yours. Schedule an appointment at any one of our 20+ easily accessible locations throughout the state, and see why we’ve been trusted for decades!